

Painless delivery, medically known as labour analgesia or epidural analgesia, is a safe and widely practised method of managing pain during childbirth. It involves administering a local anaesthetic into the epidural space of the lower back, effectively reducing or eliminating pain in the lower body while keeping the mother fully awake, alert, and able to actively participate in the birthing process.
Unlike what many believe, painless delivery does not mean a surgical or caesarean birth. In the vast majority of cases, women who opt for epidural analgesia deliver vaginally — naturally and safely — just without the intense pain that labour can bring.
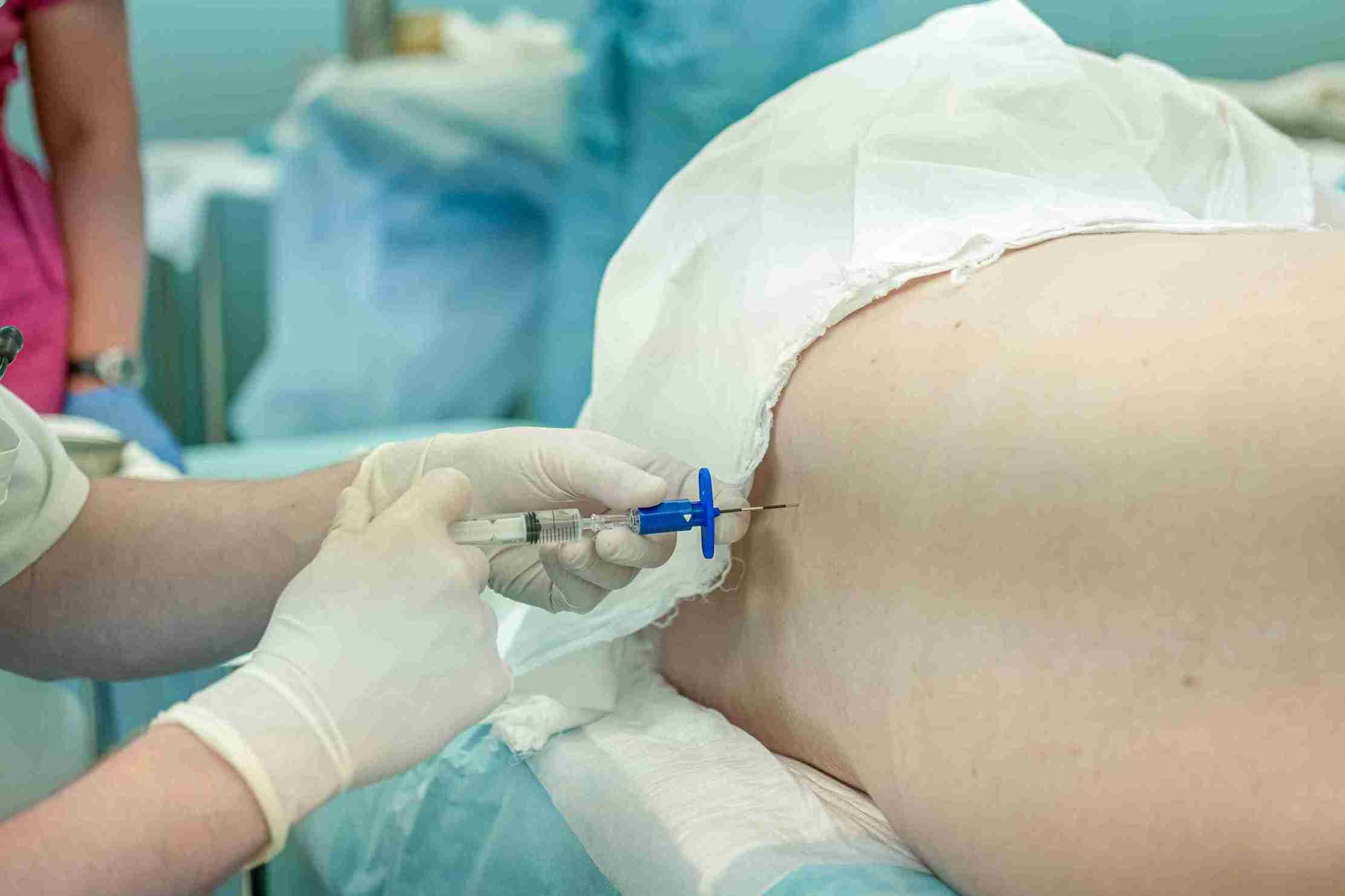
An epidural is administered by a trained anaesthesiologist once active labour begins (typically when the cervix has dilated to 3–4 cm). Here is a simple breakdown of the process:
• A small area on the lower back is cleaned and numbed with local anaesthetic.
• A thin, hollow needle is inserted into the epidural space between two vertebrae.
• A fine plastic catheter (tube) is threaded through the needle, which is then removed.
• Anaesthetic medication is delivered continuously or on demand through this catheter.
• Pain relief typically sets in within 10–15 minutes.
The catheter remains in place throughout labour, so additional doses can be given if needed. You remain conscious, can feel pressure and the urge to push, but the sharp, overwhelming pain is significantly reduced or eliminated.
Epidural analgesia is suitable for most healthy women in labour. It is particularly recommended for:
• Women with a low pain threshold or high anxiety about childbirth.
• Prolonged or difficult labour.
• Women with certain medical conditions, such as hypertension or heart disease, for whom pain management reduces strain on the body.
• First-time mothers who may have longer labours.
• Women who want to remain fully conscious and present during delivery.
Your obstetrician and anaesthesiologist will assess your health history, current medications, and the progress of your labour to determine whether it is the right choice for you.
Why Many Women Choose Epidural Analgesia
✓ Significant reduction or elimination of labour pain.
✓ Allows the mother to rest and conserve energy during long labours.
✓ Reduces stress hormones, which can actually improve blood flow to the baby.
✓ Provides a calmer, more controlled birthing environment.
✓ Can be converted to anaesthesia for a C-section if needed, without a separate procedure.
✓ Allows the mother to be fully present and participate in the birth experience.
✓ Reduces risk of trauma and birth-related PTSD.
There are many misconceptions surrounding painless delivery. Let us address the most common ones:
Myth 1: Epidurals always lead to a C-section
Fact: Research has shown that epidurals do not increase the likelihood of a C-section. In fact, most women who choose an epidural go on to have a vaginal delivery.
Myth 2: Epidurals harm the baby
Fact: Modern epidural medications are used in very low concentrations. The amount that reaches the baby through the placenta is minimal and considered safe.
Myth 3: You won't be able to push effectively
Fact: While sensation is reduced, most women can still feel the pressure and urge to push. Your medical team guides you through the process effectively.
Myth 4: Epidurals cause permanent back pain
Fact: There is no scientific evidence to suggest that epidurals cause long-term back pain. Some women may experience mild soreness at the injection site, but this is temporary and usually settles within a few days.
Like all medical procedures, epidurals carry some risks. However, serious complications are rare when performed by trained professionals. Possible side effects include:
• Temporary drop in blood pressure (managed with IV fluids and medications).
• Mild headache (occurs in fewer than 1% of cases).
• Temporary itching or shivering.
• Difficulty urinating (a catheter may be used).
• In rare cases, incomplete pain relief that requires adjustment.
At our facility, continuous monitoring of both mother and baby ensures any changes are detected and managed immediately. Your safety is always our highest priority.
"The decision to opt for painless delivery is deeply personal. My goal is to ensure every patient has accurate information, compassionate care, and the freedom to make the choice that is right for her and her baby. You are not 'taking the easy way out' — you are making an informed, courageous decision for yourself and your child."
If you are planning your delivery and wish to explore your pain management options, I encourage you to schedule a prenatal consultation. Together, we will create a personalised birth plan that reflects your values, medical history, and preferences.
Dr. Aparna Singhal
Consultant Obstetrician & Gynaecologist | Maternal & Foetal Health Specialist

Want to consult the best gynecologists in India? Please find the links below.
Want to consult the best Maternity Packages in India? Please find the links below.

Painless delivery, medically known as labour analgesia or epidural analgesia, is a safe and widely practised method of managing pain during childbirth. It involves giving a local anaesthetic into the epidural space of the lower back, effectively reducing or eliminating pain in the lower body while keeping the mother fully awake, alert, and able to participate actively in the birthing process. Importantly, painless delivery does not mean a caesarean birth; the vast majority of women who opt to deliver vaginally, naturally and safely.

An epidural is administered by a trained anaesthesiologist once active labour begins. A small area on the lower back is cleaned and numbed, after which a thin hollow needle is inserted into the epidural space between two vertebrae. A fine plastic catheter is threaded through the needle, and anaesthetic medication is delivered continuously or on demand through this catheter. Pain relief typically sets in within 10–15 minutes. The catheter remains in place throughout labour, so additional doses can be given as needed. The mother remains conscious, can feel pressure and the urge to push, but the sharp, overwhelming pain is significantly reduced or eliminated.

An epidural is typically administered once active labour begins, specifically when the cervix has dilated to 3 to 4 cm. Your obstetrician and anaesthesiologist will assess your health history, current medications, and the progress of your labour to determine the most appropriate timing for administering the epidural. It is always best to discuss your pain management preferences with your doctor well in advance so that a personalised birth plan can be created.

Epidurals do not slow labour. It does not increase the risk of a C-section, and the vast majority of women with epidurals deliver vaginally. In fact, one of the key benefits highlighted is that epidural analgesia allows the mother to rest and conserve energy during long labours, reduces stress hormones, which can improve blood flow to the baby, and provides a calmer, more controlled birthing environment. Consulting your doctor for personalised guidance is always recommended.